For many years, patients experiencing lingering symptoms long after treatment for Lyme disease often found themselves facing skepticism, both from the medical community and broader public. These individuals reported chronic fatigue, joint pain, cognitive difficulties, and neurological issues, even after completing standard antibiotic therapies. While these symptoms were real to patients, the concept of “chronic Lyme disease” remained contentious in the world of medicine. Today, however, there is a noticeable shift in how the condition is being acknowledged and addressed by healthcare professionals.
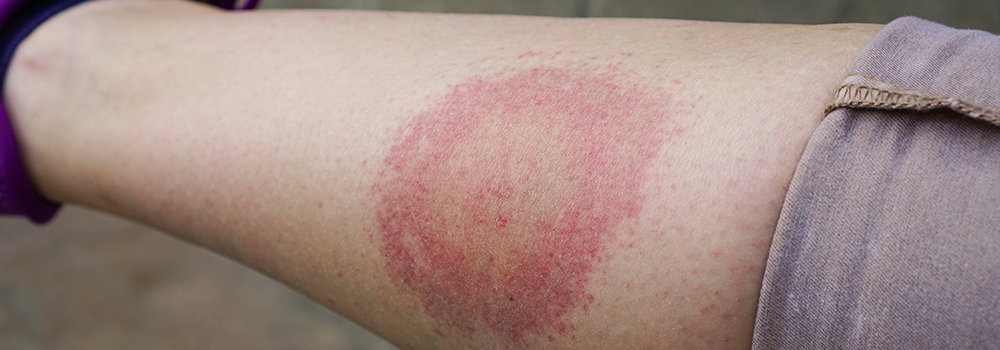
Lyme disease, caused by the bacterium Borrelia burgdorferi and transmitted through the bite of infected blacklegged ticks, is the most common vector-borne disease in the United States. Early symptoms typically include fever, fatigue, headache, and a characteristic skin rash. When caught early, the illness is generally treatable with antibiotics. However, for a notable portion of individuals, symptoms do not completely disappear after treatment. These persistent symptoms have fueled decades of debate about what is now being termed «Post-Treatment Lyme Disease Syndrome» (PTLDS).
The term PTLDS is becoming more popular among healthcare professionals because it separates the diagnosis from the disputed implications tied to «chronic Lyme disease» and recognizes that some patients do experience prolonged issues. In recent times, there has been an increase in the number of physicians who are accepting the notion that these complications after treatment deserve medical recognition and proactive care, instead of being disregarded or considered psychosomatic.
One contributing factor to the evolving perspective is the accumulation of patient-reported data and clinical studies suggesting that something more complex is happening in the body post-infection. Researchers are exploring various theories, including immune system dysregulation, lingering bacterial fragments triggering inflammation, or even the potential role of co-infections transmitted by ticks. While no single explanation has yet gained universal acceptance, the mounting evidence has opened the door for further inquiry.
Another reason for this shift in attitude is the increased visibility of Lyme disease itself. With climate change expanding the habitat of ticks, cases have surged in regions previously considered low risk. More people, including physicians and public health officials, now know someone affected by persistent Lyme-related issues, lending the condition a greater degree of legitimacy and urgency.
The traditional approach to Lyme disease treatment focuses on a few weeks of antibiotics, which work well for many but not all patients. For those with lingering symptoms, frustration often builds when test results show no remaining infection and doctors struggle to offer effective relief. This dynamic has led to the rise of a medical gray zone, where patients find themselves bouncing between specialists or turning to alternative treatments outside of mainstream medicine. Unfortunately, this lack of consistent medical guidance has sometimes left patients vulnerable to unproven therapies or even medical exploitation.
Recognizing these gaps, certain healthcare organizations are starting to establish specialized centers devoted to tick-borne diseases and ongoing Lyme symptoms. These initiatives seek to provide a more holistic approach to care, integrating neurology, immunology, and rehabilitation into their treatment strategies. Moreover, they prioritize acknowledging patient experiences and affirming their symptoms, even when conventional diagnostic methods are insufficient.
Yet, a number of areas within the medical community continue to resist this change. Doubts persist regarding whether the continued symptoms are a direct consequence of Lyme disease or stem from different illnesses or psychological reactions. Those questioning the «chronic Lyme» designation claim that it might result in misdiagnosis, guiding patients toward redundant treatments or overlooking other health problems. On the other hand, advocates for wider acknowledgment argue that ignoring ongoing symptoms leaves patients without assistance, which can frequently exacerbate their condition due to stress, prolonged diagnosis, or mental fatigue.
Insurance coverage is one more challenge. Numerous health plans restrict their coverage to brief antibiotic treatments and do not offer reimbursement for prolonged therapies or integrated medical care, citing a lack of sufficient evidence. As awareness of PTLDS increases and new research projects gain financial support, it is possible that future medical guidelines will adapt to more accurately address the requirements of these patients and enhance access to care.
Central to the situation is an increasing realization that complicated conditions such as post-treatment Lyme disease do not always align neatly with conventional diagnostic categories. Similar to how the medical community has gradually grasped the persistent impacts of COVID-19, there is a growing acknowledgment that infectious illnesses can occasionally result in enduring health issues that persist far beyond the end of the acute phase of the infection.
At the same time, individuals with lingering symptoms following Lyme therapy persist in searching for explanations, frequently navigating through a challenging path of advocacy, experimentation, and disjointed healthcare. The continual advancement in medical comprehension brings a ray of optimism—not just for acknowledgment, but also for more efficacious treatments, amplified research funding, and an increased focus on comprehensive patient care.
As awareness of Lyme disease expands and research delves further into its enduring effects, the distinction between skepticism and diagnosis might soon become less distinct. This transition is a crucial move towards establishing a more empathetic, knowledgeable, and scientifically-based method for addressing the needs of those whose struggles have long been overlooked.